
Understanding the Ramifications of Heat in Work Environments
Non-weather dependent hot work environments are created by the heat generated and/or contained within the environment, due to the task being performed, or both.
- By Iris Floyd
- Jun 01, 2016
There are three types of hot work environments: 1) weather dependent—outdoor or indoor environments affected by the weather, 2) non-weather dependent—those environments due to the nature or place of the work to be performed, and 3) a combination of both—when the non-weather dependent environment becomes part of the weather dependent environment.
The hot work environment is only one contributing factor leading to heat illnesses in healthy workers. The degree of physical effort and dehydration are also two major contributing factors to heat-related illnesses.
Weather Dependent Hot Work Environments
Heat, humidity, and direct sunlight contact are three factors presented by Mother Nature that are beyond human control. It is not enough to understand the significance of hot temperatures on the worker; one must also consider the humidity and the increase in overall temperatures when work is done in direct sunlight.
The human body can withstand higher temperatures when humidity is low because body sweat evaporates quickly to cool the body. As humidity goes up, the air becomes less absorbent and the ability of the body to cool itself through sweat evaporation decreases. Any person working in hot weather when humidity is high is at a higher risk for developing a heat illness than when humidity is low.
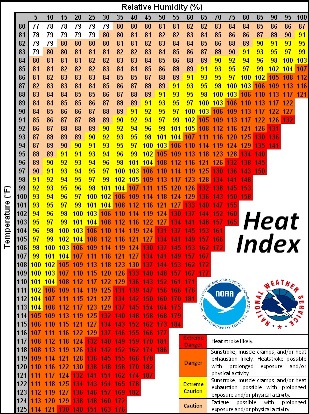
You can link to the National Weather Service Heat Index Calculator and find the heat index for the specific temperature and humidity for any weather-related work environment at any time: http://www.wpc.ncep.noaa.gov/html/heatindex.shtml
The temperatures in the heat index chart above are "air" temperatures, which are taken in the "shade." Direct sunlight contact will raise the temperature index by as much as 15 degrees F.
Just as direct sunlight contact with innate surfaces raises those surface temperatures, it raises the temperature of the human body. For example, the surface of a black car in direct sunlight will be hotter than the surface of a white car in direct sunlight, and both will be hotter than the temperature of the air. Just as surface heat is transferred to the inside of each car, the heat of direct sunlight on the surface of the human body is transferred through the skin to warm the body’s core. Also, as with the white car, the heat effect can be lessened with the use of light colored, lightweight clothing.
Non-Weather Dependent Hot Work Environments
Non-weather dependent hot work environments are created by the heat generated and/or contained within the environment, due to the task being performed, or both. These include places where heat-generating equipment is used, such as bakeries, foundries, etc., or workers are wearing heavy, protective clothing that holds in heat, such as that worn by welders, hazmat crews, firefighters, and others.
Hot work environments that are created by the nature of the job itself require frequent monitoring of the worker. Take for example, a worker making repairs on a very large, hot, metal tank. The radiant heat from the tank itself may literally pull moisture away from the worker's body. Because the worker's clothes do not show significant signs of sweating, to others, the worker may not appear to be hot, when in fact his body temperature may have risen to a dangerous level. Dehydration in this type of situation can also rapidly occur.
Combination Hot Work Environments
When the work to be performed creates a hot work environment and this work is done in a hot weather environment, the chances of a worker developing a serious heat illness become greater. Take for example, hazmat crews working an outdoor chemical spill in full protective gear. Even with cooling vests worn under their suits, workers generally work on a 30-minute rotation: 30 minutes of work followed by 30 minutes of hydration and rest in a cool environment, usually an air-conditioned trailer or vehicle. This cooling time allows for full heat recovery before the next rotation begins.
The hazmat suits create a closed, non-weather related work environment that heats up due to body heat and is exacerbated by weather-related heat. If the weather is very hot, shortened work periods may be required.
Exertional Heat Stress
The term "work environment" implies physical exertion. Physical exertion is required to perform any task. It is the degree to which it is required in performing the task that becomes a factor in heat illnesses. A desk clerk, even in a hot work environment, is not likely to be at risk of a serious heat illness. A laborer performing physical tasks in that same hot work environment would be at risk according to the degree of his physical exertion. It is this physical exertion that introduces another factor in heat illnesses known as Exertional Heat Stress, or EHS.
Even on a day when environmental temperatures are pleasant and humidity is low, a worker can become overheated from strenuous, physical work. Just as in athletes, the duration of the physical effort also affects body heat. The greater the physical effort and the greater the duration of the physical effort, the greater the body heat generated. Add EHS to any type of hot work environment and additional monitoring for heat illnesses is required, especially if the work is in direct sunlight or humidity is also high.
Dehydration
Dehydration is the loss of water from the body, which occurs mainly through urination and sweat. It almost always accompanies heat illnesses.
The human body is around 70 percent water, with the brain being made up of 73 percent water. As dehydration progresses, the brain loses the water it needs to function at its best. As body heat rises, the body produces sweat for evaporation to cool itself. Too much sweating causes dehydration, which in turn lessens brain function; decreases the body’s ability to cool itself; lessens toxins removal; causes low levels of sodium, potassium, chloride, and other needed minerals; and deleteriously affects other body functions.
Staying hydrated only requires the worker to regularly drink cool fluids, preferably water and electrolyte-replacing drinks. Hydration isn't only easy, it is also essential on all levels for keeping workers safe and efficient in their tasks.
Stopping Heat Stroke
A hot environment, physical exertion, and dehydration can lead to heat illnesses that require immediate attention. Heat stroke is 100 percent preventable. Every employer and employee subject to a hot work environment should know the signs and symptoms of heat illnesses and know how to prevent and treat them.
It is important to understand that heat stroke occurs when body temperature reaches 104 degrees F. Because the body can no longer adequately cool itself, the body temperature will very likely continue to rise, and without immediate intervention, death can occur shortly afterward. When heat stroke occurs, the first 10 minutes are critical for preventing brain and other organ damage, and death. Lowering the body temperature becomes essential for survival. The quicker the body temperature is lowered, the less likely damage to the brain and other body organs will occur.
While hydration is also needed, if the person is in heat stroke, he or she may not be able to drink. Once the body temperature is down and the person can drink, start giving cold fluids.
To get the person's temperature down quickly, move the person away from the heat source. If in the sun, shade the person and immediately apply cold therapy. Cold therapy is any method of lowering body temperature by applying continuous cold to the body in any safe form—ice, ice water, cold water, cool water, cold blankets, cold packs, and vigorous fanning. In short, by whatever cooling application is available. Moving the person away from the heat source, shading, and waiting for emergency medical services to arrive is not an option to prevent or treat heat stroke. Cooling the person down is the only option to prevent and treat heat stroke.
Whenever heat stress has escalated to heat exhaustion, medical services should be called and on-site cooling of the person should immediately begin. Heat stroke can occur suddenly, without any symptoms of heat exhaustion. As previously stated, heat stroke is 100 percent preventable. When a heat illness occurs on the work site, the single over-riding rule is "cool down and hydrate."
Don't wait for medical services to begin cold therapy. Doing so could result in death. If every employer and employee learned and executed "cool down and hydrate" by any means possible while waiting on medical services, heat stroke in the work place could be eliminated.
Heat Illness Symptoms
Heat Stress
- Cramps in the hands, calves, feet, or stomach
- Light headedness, dizziness
Cool down and hydrate.
Heat Exhaustion
- Fatigue
- Nausea
- Headache
- Thirst
- Heavy sweating
- Cool, moist skin, which may have goose bumps
- Cold, clammy skin
- Profuse sweating
- Muscle aches or cramps
- Light headedness, dizziness, or fainting
- Weakness
- Confusion or anxiety
- Shallow breathing
- Slowed or weakened heartbeat
- Irritability
Seek medical care immediately. Cool down and hydrate.
Heat Stroke
- Nausea
- Vomiting
- Headache
- Confusion, delirium
- Loss of consciousness
- Hot, dry skin
- Flushed skin (reddened)
- Excessive sweating
- Rapid heart rate
- Short, rapid breaths
- Convulsions
- High temperature (104F or higher)
Seek medical care immediately. Cool down and hydrate. Any delay could be fatal!
This article originally appeared in the June 2016 issue of Occupational Health & Safety.